Congenital Pseudarthrosis
Editors: Frassica, Frank J.; Sponseller, Paul D.; Wilckens, John H.
Title: 5-Minute Orthopaedic Consult, 2nd Edition
Copyright ©2007 Lippincott Williams & Wilkins
> Table of Contents > Congenital Pseudarthrosis
Congenital Pseudarthrosis
Paul D. Sponseller MD
Description
-
Congenital pseudarthrosis is a rare
defect of the distal tibia (at the junction of the middle 1/3 and
distal 1/3) in which the bone is cystic and bowed and eventually
fractures.-
The bone is dysplastic from birth.
-
The deformity often increases with age.
-
The abnormality may not be noticed unless anterior bowing becomes prominent or fracture occurs.
-
It has no spontaneous healing potential, and it may require surgery to attempt union.
-
Multiple surgical procedures sometimes are required.
-
It is almost always unilateral.
-
After maturity, the bone behaves more normally.
-
-
About 1/2 of cases are associated with NF; in those cases, other skeletal findings may be present.
-
Congenital pseudarthrosis also may occur in other bones, such as the forearm and clavicle.
-
These occurrences are even rarer than those in the tibia.
-
Other sites are not affected concurrently in the patient with tibia pseudarthrosis.
-
Congenital pseudarthrosis of the clavicle affects only the right side unless the patient has dextrocardia.
-
-
Classification (1–3):
-
Congenital pseudarthrosis is associated in some cases with NF.
-
Isolated congenital pseudarthrosis has been subclassified (1–3) into 3 types:
-
Dysplastic
-
Cystic
-
Sclerotic
-
-
-
Synonyms: Congenital kyphoscoliotic tibia; Dysplastic tibia
Epidemiology
Males and females are affected equally with all types of congenital pseudarthroses.
Incidence
~1 per 100,000–1 per 200,000 in the population are affected (3,4).
Risk Factors
-
NF
-
Bowing of the tibia
Genetics
-
NF is an autosomal dominant disorder.
-
Its gene is located on the long arm of chromosome 17, and normally codes for a tumor suppressor, neurofibromin.
-
Otherwise, congenital pseudarthrosis in the absence of NF is not an inherited disorder.
Etiology
-
The cause is unknown.
-
Fracture usually occurs with minor or unrecognized trauma.
-
The distal segment of the tibia is in the most poorly vascularized region of the bone
-
NF tissue is not found in pseudarthrosis.
Associated Conditions
NF
Signs and Symptoms
-
Signs:
-
Increasing anterior and lateral bow of distal tibia (Fig. 1)
-
Mild limp
-
Possible signs of NF may be present, such as:
-
>5 café-au-lait spots
-
Subcutaneous NF
-
Scoliosis
-
-
In pseudarthrosis of the clavicle, bump in the right midclavicle with clicking
-
Mild leg-length difference possible
-
-
Symptom:
-
Minimal to no pain
-
Physical Exam
-
Inspect for signs of NF.
-
Assess for limb-length discrepancy and stability.
-
Assess the foot for size, stability, and plantigrade status.
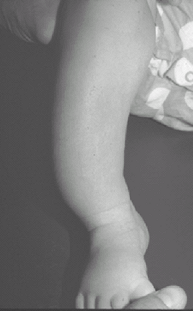 Fig.
Fig.
1. Clinical appearance of anterolateral bow of the tibia secondary to
congenital pseudarthrosis. Note the distal location of the bow.
Tests
Lab
No characteristic laboratory findings are noted, and no special tests are indicated routinely.
Imaging
-
Radiography:
-
Plain AP and lateral films display the lesion in the distal tibia and fibula.
-
-
MRI is not routinely indicated.
-
Even before fracture, 1 or both of the following signs may be evident:
-
Cyst formation and sclerosis in the lesion
-
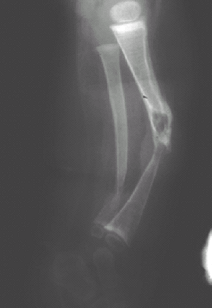
Local tapering (Fig. 2)
-
-
Once the fracture appears, it may be characterized as atrophic or hypertrophic.
-
A search for NF should be conducted, but the full-blown signs of NF may not appear until later in the 1st decade of life.
-
If vascularized bone grafting is indicated, a preoperative angiogram is useful for showing vascular anatomy.
Pathological Findings
-
The pseudarthrosis resembles that of any other cause.
-
A thick cuff of hamartomatous tissue encircles the tibia.
-
This cuff contains inactive fibroblasts, with no findings of NF such as Schwann cells, axons, or perineural cells.
Differential Diagnosis
-
Ossifying fibroma: A multiple cystic lesion affecting the anterior cortex of the tibia in older children
-
Fibrous dysplasia: May produce bowing, but rarely fracture
-
Posteromedial bow of the tibia: Benign, self-correcting bow in the same region of the tibia but in the opposite direction
-
Focal fibrocartilaginous dysplasia: Rare, usually self-correcting bow of the proximal tibial metaphysis that rarely fractures
-
Nonunion after fracture or osteotomy of the distal tibia
![]() Fig. 2. Lateral radiograph of the tibia showing the tapering and cyst formation typical of congenital pseudarthrosis.
Fig. 2. Lateral radiograph of the tibia showing the tapering and cyst formation typical of congenital pseudarthrosis.
P.89
General Measures
-
The leg should be splinted and monitored to rule out increasing deformity.
-
If the lesion has not fractured, a brace should be provided for protection.
-
If the lesion has fractured, surgery always is required.
Special Therapy
Physical Therapy
Physical therapy is not necessary.
Medicatio (Drugs)N
-
Medications do not affect the success of treatment.
-
A recent article has suggested that rhBMP2 does not seem to improve the results of surgical treatment (5).
Surgery
-
Intramedullary nail with bone graft: The nail is left in place until maturity (6,7).
-
Ilizarov treatment: Distraction and compression of the fracture site stimulates a healing response (4).
-
Free vascularized fibula graft: A segment
of living, normal fibula with its blood supply is transferred to
increase chances of success (8). -
As a last resort, if many different
treatments do not succeed, Syme amputation through the ankle may be
elected by the family to allow the child to proceed with physical
activities (4).
Prognosis
-
Good: 80–90% may heal (4–8).
-
Refracture may occur even after union.
-
Refracture rate and nonunion rate decline after puberty (3).
Complications
-
Nonunion of defect after surgical procedure
-
Angular deformity because of the small size and bowing of the distal fragment (9)
-
Recurrence of fracture, even months to years after apparent healing
-
Foot and ankle stiffness
-
Limb-length inequality
Patient Monitoring
The patient should be seen every 3–6 months to rule out progressive bowing and leg-length inequality and to check brace fit.
References
1. Boyd HB, Sage FP. Congenital pseudarthrosis of the tibia. J Bone Joint Surg 1958;40A:1245–1270.
2. Boyd HB. Pathology and natural history of congenital pseudarthrosis of the tibia. Clin Orthop Relat Res 1982;166:5–13.
3. Morrissy RT, Riseborough EJ, Hall JE. Congenital pseudarthrosis of the tibia. J Bone Joint Surg 1981;63B:367–375.
4. Schoenecker
PL, Rich MM. The lower extremity. In: Morrissy RT, Weinstein SL, eds.
Lovell and Winter’s Pediatric Orthopaedics, 6th ed. Philadelphia:
Lippincott Williams & Wilkins, 2006:1157–1211.
PL, Rich MM. The lower extremity. In: Morrissy RT, Weinstein SL, eds.
Lovell and Winter’s Pediatric Orthopaedics, 6th ed. Philadelphia:
Lippincott Williams & Wilkins, 2006:1157–1211.
5. Lee
FYI, Sinicropi SM, Lee FS, et al. Treatment of congenital
pseudarthrosis of the tibia with recombinant human bone morphogenetic
protein-7 (rhBMP-7). A report of five cases. J Bone Joint Surg 2006;88A:627–633.
FYI, Sinicropi SM, Lee FS, et al. Treatment of congenital
pseudarthrosis of the tibia with recombinant human bone morphogenetic
protein-7 (rhBMP-7). A report of five cases. J Bone Joint Surg 2006;88A:627–633.
6. Dobbs
MB, Rich MM, Gordon JE, et al. Use of an intramedullary rod for
treatment of congenital pseudarthrosis of the tibia. A long-term
follow-up study. J Bone Joint Surg 2004;86A:1186–1197.
MB, Rich MM, Gordon JE, et al. Use of an intramedullary rod for
treatment of congenital pseudarthrosis of the tibia. A long-term
follow-up study. J Bone Joint Surg 2004;86A:1186–1197.
7. Dobbs
MB, Rich MM, Gordon JE, et al. Use of an intramedullary rod for the
treatment of congenital pseudarthrosis of the tibia. Surgical
technique. J Bone Joint Surg 2005;87A:33–40.
MB, Rich MM, Gordon JE, et al. Use of an intramedullary rod for the
treatment of congenital pseudarthrosis of the tibia. Surgical
technique. J Bone Joint Surg 2005;87A:33–40.
8. Weiland AJ, Weiss APC, Moore JR, et al. Vascularized fibular grafts in the treatment of congenital pseudarthrosis of the tibia. J Bone Joint Surg 1990;72A:654–662.
9. Kristiansen LP, Steen H, Terjesen T. Residual challenges after healing of congenital pseudarthrosis in the tibia. Clin Orthop Relat Res 2003;414:228–237.
Codes
ICD9-CM
733.82 Congenital pseudarthrosis
Patient Teaching
-
The family should be educated about the
natural history of the lesion—the propensity for fracture, the need for
bracing, the tendency to nonunion, treatment options, improvement in
biology (increased chance of healing and less likelihood of refracture)
after puberty. -
With this knowledge, they will be more understanding of the multiple procedures sometimes needed for healing.
-
Rough play should be avoided as much as possible.
-
Prevention of fracture or refracture by use of a brace is common practice.
FAQ
Q: What is the cause of congenital pseudarthrosis of the tibia?
A: The cause is unknown.
Q: Which of the surgical treatments listed is better?
A: No superiority of one over the other is proven. Treatment choice depends on the experience and preference of the surgeon.