Genu Valgum (Knock-Knee)
Editors: Frassica, Frank J.; Sponseller, Paul D.; Wilckens, John H.
Title: 5-Minute Orthopaedic Consult, 2nd Edition
Copyright ©2007 Lippincott Williams & Wilkins
> Table of Contents > Genu Valgum (Knock-Knee)
Genu Valgum (Knock-Knee)
Paul D. Sponseller MD
Description
-
Genu valgum, or knock-knee, is a normal phase of development in children 2–4 years old.
-
Girls normally have slightly more valgus of the knee than do boys.
-
The valgus straightens to achieve the adult position by 6–7 years of age (1,2).
-
Rickets, trauma, and genetic disorders also may cause genu valgum.
-
Some patients have an idiopathic valgus,
not resulting from any of the foregoing disorders, that falls outside
the normal limits and persists beyond 10 years of age. -
Areas affected include the distal femoral and proximal tibial growth plates.
Epidemiology
Incidence
-
The condition is rare.
-
Pathologic valgus occurs in <1 per 1,000 (2).
Prevalence
-
It occurs in young children, usually 3–11 years old (1).
-
Physiologic genu valgum is more common in females than in males.
Risk Factors
-
Family history of genu valgum
-
Proximal tibia metaphysic fracture in
children (Cozen fracture); asymmetric overgrowth occurs and deformity
is possible (parents should be warned about this possibility).
Genetics
-
Many forms of rickets are transmitted genetically.
-
Idiopathic valgus may be transmitted in families.
Etiology
-
Physiologic genu valgum (Fig. 1)
-
Metabolic disorder (e.g., rickets)
-
Steroid dependence
-
Proximal tibia fracture (3,4)
-
Skeletal dysplasias
-
Chromosome disorders (e.g., Klinefelter syndrome)
Associated Conditions
-
Proximal tibia fracture
-
Pseudoachondroplasia
-
Renal osteodystrophy
-
Metaphyseal dysplasia
-
Rickets
-
Down syndrome
Signs and Symptoms
-
Parental concern about the appearance of the child’s legs is the most common reason for presentation.
-
It is usually asymptomatic.
-
The knees usually are not painful in
childhood but the physical appearance is sometimes bothersome;
occasionally, valgus knees are associated with patellar discomfort. -
In adulthood, valgus knees are more likely to produce arthritic symptoms outside of the joint.
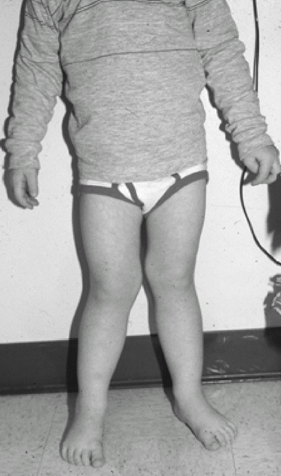 Fig. 1. This 3-year-old had typical physiologic genu valgum. It resolved with growth within 1 year.
Fig. 1. This 3-year-old had typical physiologic genu valgum. It resolved with growth within 1 year.
Physical Exam
-
Measure the ROM of the knee.
-
Determine and plot height and weight percentiles for the patient’s age.
-
Measure the angle between the tibia and the femur with a goniometer.
-
Measure the distance between the ankles when the knees are touching (intermalleolar distance).
-
Assess the alignment and ROM in the adjacent hip and ankle.
-
Check the rotation of the limb and the gait.
-
Check the collateral ligaments of the knee for laxity.
Tests
Lab
-
Serum levels of calcium, phosphate,
alkaline phosphatase, urea nitrogen, and creatinine should be measured
if rickets or a metabolic problem is suspected. -
The most common type of rickets in developed countries is familial hypophosphatemic rickets.
-
If rickets is to be evaluated, check vitamin D levels (25-hydroxy and 1,25-dihydroxy) as well as the other parameters.
Imaging
-
Imaging of genu valgum, which is thought
to be physiologic, is unnecessary for children <6 years old unless
the patient has an asymmetric deformity or a pathologic condition is
suspected. -
An AP view of the lower extremity from the hip to ankle obtained while the patient is standing should be the 1st imaging study.
-
The knee should be pointing straight ahead.
-
The film cassette should be long enough to accommodate the entire extremity.
-
The femorotibial angle should be measured, and the site of the deformity should be identified as femoral, tibial, or both.
-
Differential Diagnosis
-
The main differential diagnosis is to determine whether the condition is physiologic or pathologic.
-
Physiologic genu valgum occurs without underlying rickets, dysplasia, or other known cause.
-
The most common skeletal dysplasias
causing valgus are metaphyseal dysplasia and pseudoachondroplasia, as
well as multiple osteochondromas.
P.153
General Measures
-
Physiologic valgus:
-
No treatment is indicated for physiologic genu valgum in patients <7 years old.
-
If the deformity persists after 7 years
of age, hemiepiphysiodesis (at age 11–12 years) may be considered to
achieve normal alignment.-
Epiphysiodesis consists of slowing or stopping the growth plate on the medial side to allow the lateral side to catch up.
-
This relatively simple procedure does not substantially weaken the bone and allows early weightbearing.
-
-
-
Pathologic valgus:
-
For metabolic disorders, including renal osteodystrophy, the underlying condition should be treated.
-
Bracing has not been effective in preventing or reversing the deformity.
-
Single- or multiple-level osteotomy may be necessary to correct the deformity; medical control of the disease is needed first.
-
Usually, therapy is directed by a renal or endocrine specialist.
-
-
Fracture:
-
Follow-up of proximal tibia fracture should extend for several years after the injury (3).
-
Early tibial osteotomy should be avoided because of the high incidence of recurrence of valgus deformity (3).
-
If an unacceptable degree of valgus remains after 1–2 years follow-up, hemiepiphysiodesis or osteotomy may be indicated (5,6).
-
-
Dysplasia:
-
Children with pseudoachondroplasia and metaphyseal dysplasias are likely to develop genu valgum.
-
Osteotomy may be necessary to correct the deformity.
-
Activity
No activity restrictions are necessary.
Special Therapy
Physical Therapy
Not indicated, because therapy and exercises cannot affect the growth of the limb
Surgery
-
2 types of surgery commonly are used to correct valgus deformity when it persists: Hemiepiphysiodesis and varus osteotomy.
-
Epiphysiodesis aims to achieve satisfactory mechanical alignment at the end of growth.
-
Proximal tibia osteotomy should be considered if epiphysiodeses is not feasible.
-
Osteotomy involves a more difficult
recovery period than epiphysiodesis because, in the former procedure,
the bone is divided completely.
-
-
-
The overall success rate of surgery is >90%.
Prognosis
Physiologic genu valgum resolves by age 7–10 years as long as it is mild (<15°) and no metabolic problems are present.
Complications
-
Untreated genu valgum: If severe, the
patient may develop patellofemoral pain and late degenerative arthritis
from stresses on the lateral joint surface. -
Surgical complications:
-
Infection
-
Compartment syndrome
-
Recurrence of deformity or overcorrection and neurovascular injury
-
Patient Monitoring
Children with idiopathic genu valgum may be followed
every 12–24 months to determine whether the deformity is improving
before a treatment decision is made.
every 12–24 months to determine whether the deformity is improving
before a treatment decision is made.
References
1. Arazi
M, Ogun TC, Memik R. Normal development of the tibiofemoral angle in
children: a clinical study of 590 normal subjects from 3 to 17 years of
age. J Pediatr Orthop 2001;21:264–267.
M, Ogun TC, Memik R. Normal development of the tibiofemoral angle in
children: a clinical study of 590 normal subjects from 3 to 17 years of
age. J Pediatr Orthop 2001;21:264–267.
2. White GR, Mencio GA. Genu valgum in children: diagnostic and therapeutic alternatives. J Am Acad Orthop Surg 1995;3:275–283.
3. Balthazar DA, Pappas AM. Acquired valgus deformity of the tibia in children. J Pediatr Orthop 1984;4:538–541.
4. Brougham DI, Nicol RO. Valgus deformity after proximal tibial fractures in children. J Bone Joint Surg 1987;69B:482.
5. Bowen JR, Torres RR, Forlin E. Partial epiphysiodesis to address genu varum or genu valgum. J Pediatr Orthop 1992;12:359–364.
6. Ferrick MR, Birch JG, Albright M. Correction of non-Blount’s angular knee deformity by permanent hemiepiphyseodesis. J Pediatr Orthop 2004;24:397–402.
Codes
ICD9-CM
736.41 Genu valgum
Patient Teaching
Inform parents that most cases of physiologic genu valgum begin to resolve spontaneously by 7 years of age.
FAQ
Q: Is bracing indicated in genu valgum?
A:
Bracing for valgus has never been shown to be effective. It is very
cumbersome because the knee cannot bend in a corrective brace.
Bracing for valgus has never been shown to be effective. It is very
cumbersome because the knee cannot bend in a corrective brace.
Q: Is valgus a cosmetic problem or a functional one?
A: In the more severe degrees, it can impair running and increase the risk of arthritis.
