Bunion/Hallux Valgus
Editors: Frassica, Frank J.; Sponseller, Paul D.; Wilckens, John H.
Title: 5-Minute Orthopaedic Consult, 2nd Edition
Copyright ©2007 Lippincott Williams & Wilkins
> Table of Contents > Bunion/Hallux Valgus
Bunion/Hallux Valgus
Gregory Gebauer MD, MS
Description
-
A bunion is an enlargement of the medial eminence of the 1st metatarsal with soft tissue and bursal swelling.
-
Hallux valgus occurs primarily at the MTP
joint and consists of lateral deviation of the great toe with medial
deviation of the 1st metatarsal. -
Subluxation of the MTP joint often occurs.
General Prevention
Avoidance of narrow footwear
Epidemiology
-
Occurs predominantly in middle-aged to elderly women, but can be seen in adolescents and young adults
-
Females are affected more than males.
-
Occurs almost exclusively in shoe-wearing societies
Prevalence
Reported to occur in up to 33% of individuals (1)
Risk Factors
-
Heredity
-
Shoe wear
Genetics
-
May be an unidentified genetic component
-
Positive family history in 2/3 of patients
-
Hallux valgus also is seen commonly as a component of a hyperlaxity syndrome that is thought to have a genetic component.
Etiology
-
Shoes with narrow toe boxes and high heels are believed to be related to the development of hallux valgus.
-
Higher incidence in shod versus unshod
societies and increasing incidence in populations that adopt more
Westernized shoe styles (Fig. 1) (1)
-
-
Pes planus also may be a causative
factor: Part of a laxity syndrome and associated with mechanically
abnormal pressure on the 1st MTP joint secondary to a pronated gait.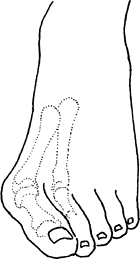 Fig. 1. A bunion is produced by an underlying imbalance of the soft tissues and extrinsic pressure.
Fig. 1. A bunion is produced by an underlying imbalance of the soft tissues and extrinsic pressure. -
Metatarsus primus varus is associated; a
strong relationship exists between an increase in the angle between the
1st and 2nd metatarsal joints and the development of hallux valgus. -
Acquired joint laxity (e.g., from rheumatoid arthritis, gout, or trauma) can contribute to the development.
-
Other miscellaneous conditions (e.g.,
amputation of another toe, severe hammering of the toes, Achilles
tendon contracture) also may be associated.
Signs and Symptoms
-
The primary symptom is pain over the medial eminence, often caused by shoe wear pressure.
-
The patient has lateral deviation of the great toe and prominence of the medial eminence.
-
The deformity may be accentuated with weightbearing.
-
When the condition is advanced, impingement by the great toe on the 2nd toe can lead to 2nd-toe pain and deformity.
-
Can be associated with pain under the 2nd metatarsal head (transfer metatarsalgia), 1st metatarsal joint pain, and arthritis.
-
Patients’ complaints often are cosmetically based and concern difficulty with shoe wear.
Physical Exam
-
Examine the sitting and standing patient.
-
Assess for Achilles tendon and
gastrocnemius contracture with the knee flexed and extended (indicated
by limited ankle dorsiflexion). -
Check motion at the ankle, subtalar, midfoot, and metatarsal joints.
-
Manually assess for increased laxity or instability of the 1st metatarsocuneiform joint with vertical shear or stress.
-
Assess the flexibility or rigidity of the hallux valgus deformity by manually reducing the alignment of the toe.
-
Pay attention to foot morphology and arch status.
-
Perform a complete neurovascular and musculoskeletal examination of the entire lower extremity.
Tests
Imaging
-
Obtain standing AP, oblique, lateral, and axial (sesamoid) foot radiographs.
-
Assess for the intermetatarsal angle,
hallux valgus angle, hallux IP angle, distal metatarsal articular
angle, and the sesamoid incongruence. -
Evaluate for joint incongruence and arthrosis, which greatly influences the treatment plan.
-
Evaluate lesser toe alignment.
-
Pathological Findings
-
2 broad categories of hallux valgus
occur, each with different entities and different pathoanatomic
features: A noncongruent joint and a congruent joint. -
Incongruent joint:
-
Multiple static and dynamic anatomic components
-
The 1st metatarsal head drifts medially (varus), thus increasing the angle between the 1st and 2nd metatarsals.
-
The sesamoid complex is held in place by
the transverse metatarsal ligament and thus becomes relatively
laterally positioned as the metatarsal head displaces medially. -
With progressive deformity, the axis of
pull for the adductor hallucis, the flexor hallucis brevis, extensor
hallucis longus, and the abductor hallucis become lateralized, which
dynamically contributes to the lateral displacement of the great toe. -
The medial joint capsule and ligaments become attenuated, whereas the lateral joint capsule and ligaments become contracted.
-
-
Congruent joint:
-
A laterally sloped articular surface is present, with no pathologic articulation, so progression of deformity is less likely.
-
Differential Diagnosis
Gout
General Measures
-
Hallux valgus should be treated initially with nonoperative measures.
-
Appropriate shoe wear is essential.
-
Pointed shoes and high heels must be avoided.
-
Lace-up styles have wider forefeet.
-
Soft leather shoes can be stretched to accommodate the bunion.
-
No stitching should be present over the medial eminence.
-
-
Numerous off-the-shelf cushions, pads, or splinting devices may alleviate pressure over the medial bunion.
-
Heel cord stretching and custom orthotic
arch support may have a role for patients with associated Achilles
contracture and pes planus (2). -
Prescription shoes, wide with increased depth, can be ordered if needed.
Special Therapy
Physical Therapy
Not usually helpful for symptom relief
Medication (Drugs)
Analgesic medications may be necessary for symptomatic control.
P.45
Surgery
-
Goals of surgery: Pain relief, correction
of the deformity, restoration of normal biomechanics, and maintenance
of adequate joint motion -
Indications for surgery:
-
Failed nonsurgical treatments
-
Worsening pain and deformity
-
Decreased function and inability to tolerate shoe wear
-
-
Contraindications for surgery:
-
Cosmetic complaints alone without symptoms
-
Vascular insufficiency
-
-
Options:
-
Multiple surgical procedures exist.
-
A decision tree for appropriate care is based on multiple factors.
-
Age
-
The angle between the 1st and 2nd metatarsal joint (normal, 9°)
-
The MTP angle (normal, 15°)
-
Congruity or incongruity of the joint
-
In the presence of degenerative joint
disease, the options are to fuse or to place a prosthesis; currently,
prosthesis technology is associated with high complication and failure
rates and is not recommended for active individuals (3). -
The presence of a rigid joint
-
-
-
Overview of surgical procedures:
-
Silver procedure:
-
Resection of the medial eminence should be used only for elderly patients.
-
Low complication rate, high recurrence rate
-
-
Modified McBride procedure (4):
-
Soft-tissue repair with resection of the
medial eminence; release of the contracted lateral joint capsule,
adductor hallucis tendon, and transverse metatarsal ligament; and
imbrication of the medial capsule -
Corrects hallux valgus angle
-
Can be used for mild deformities
-
More effective when performed with a proximal metatarsal osteotomy
-
Complications include hallux varus (overcorrection) and stiffness.
-
-
Distal metatarsal chevron osteotomy combined with a medial eminence resection and medial capsule plication (5):
-
The metatarsal head fragment is translated laterally, correcting intermetatarsal angle.
-
Appropriate for mild to moderate deformity (cannot adequately correct more severe deformities)
-
Can be complicated by malunion, osteonecrosis, or hallux varus
-
-
Metatarsocuneiform arthrodesis and distal soft-tissue correction (Lapidus procedure) (6):
-
For hallux valgus deformities with hypermobility or instability of 1st metatarsocuneiform joint
-
Corrects increased intermetatarsal angle
-
Combined with modified McBride correction at the MTP joint
-
-
Proximal metatarsal osteotomy and distal soft-tissue correction (4,7):
-
For more severe hallux valgus deformities
-
Corrects increased intermetatarsal angle
-
Numerous configurations of proximal
osteotomies have been described, including crescentic, oblique, opening
wedge, and proximal chevron osteotomies. -
Combined with modified McBride correction at the MTP joint.
-
-
MTP arthrodesis (8):
-
For severe deformities in elderly
individuals; hallux valgus with degenerative or inflammatory arthritis,
underlying spasticity, or connective tissue disorders, and as salvage
for failed surgery -
Fusion has dependable rates of pain relief and satisfaction but does result in hallux stiffness.
-
-
Resection arthroplasty (Keller) bunionectomy (9):
-
Involves removal of the medial eminence and base of the proximal phalanx
-
Appropriate only for older, sedentary patients
-
Can be associated with multiple complications, including recurrent valgus, transfer metatarsalgia, and cock-up 1st toe.
-
-
Akin phalangeal osteotomy procedure (10):
-
A medial closing wedge osteotomy of the proximal phalanx
-
For isolated hallux valgus interphalangeus or in combination with more proximal metatarsal osteotomy or fusion
-
-
Prognosis
-
Mild deformities and congruent
deformities have lower rates of progression with nonoperative
management than do severe or incongruent deformities. -
Surgical treatment with appropriate
indications and decision-making typically results in pain relief and
deformity correction in most patients.
Complications
Surgical complications include wound breakdown and
infection, recurrence of the deformity, overcorrection leading to
hallux varus, malunion or nonunion of osteotomy or fusion procedures,
joint stiffness, neuroma, and transfer metatarsalgia.
infection, recurrence of the deformity, overcorrection leading to
hallux varus, malunion or nonunion of osteotomy or fusion procedures,
joint stiffness, neuroma, and transfer metatarsalgia.
References
1. Sim-Fook L, Hodgson AR. A comparison of foot forms among the non-shoe and shoe-wearing Chinese population. J Bone Joint Surg 1958;40A:1058–1062.
2. Torkki
M, Malmivaara A, Seitsalo S, et al. Surgery vs orthosis vs watchful
waiting for hallux valgus: a randomized controlled trial. JAMA 2001;285:2474–2480.
M, Malmivaara A, Seitsalo S, et al. Surgery vs orthosis vs watchful
waiting for hallux valgus: a randomized controlled trial. JAMA 2001;285:2474–2480.
3. Shereff MJ, Jahss MH. Complications of silastic implant arthroplasty in the hallux. Foot Ankle 1980;1:95–101.
4. Mann
RA, Rudicel S, Graves SC. Repair of hallux valgus with a distal
soft-tissue procedure and proximal metatarsal osteotomy. A long-term
follow-up. J Bone Joint Surg 1992;74A:124–129.
RA, Rudicel S, Graves SC. Repair of hallux valgus with a distal
soft-tissue procedure and proximal metatarsal osteotomy. A long-term
follow-up. J Bone Joint Surg 1992;74A:124–129.
5. Trnka
HJ, Zembsch A, Easley ME, et al. The chevron osteotomy for correction
of hallux valgus: Comparison of findings after two and five years of
follow-up. J Bone Joint Surg 2000;82A:1373–1378.
HJ, Zembsch A, Easley ME, et al. The chevron osteotomy for correction
of hallux valgus: Comparison of findings after two and five years of
follow-up. J Bone Joint Surg 2000;82A:1373–1378.
6. Sangeorzan BJ, Hansen ST, Jr. Modified Lapidus procedure for hallux valgus. Foot Ankle 1989;9:262–266.
7. Chiodo CP, Schon LC, Myerson MS. Clinical results with the Ludloff osteotomy for correction of adult hallux valgus. Foot Ankle Int 2004;25:532–536.
8. Coughlin MJ, Grebing BR, Jones CP. Arthrodesis of the first MTP joint for idiopathic hallux valgus: intermediate results. Foot Ankle Int 2005;26:783–792.
9. Vallier GT, Petersen SA, LaGrone MO. The Keller resection arthroplasty: a 13-year experience. Foot Ankle 1991;11:187–194.
10. Frey C, Jahss M, Kummer FJ. The Akin procedure: an analysis of results. Foot Ankle 1991;12:1–6.
Additional Reading
Coughlin MJ. Hallux valgus. J Bone Joint Surg 1996;78A:932–966.
Codes
ICD9-CM
-
727.1 Bunion
-
735.0 Hallux valgus
-
754.52 Metatarsus primus varus
Patient Teaching
Activity
Once the patient is no longer in the perioperative period, few limitations are placed on activity.
Prevention
The most important factor in prevention is the use of
proper shoe wear and the avoidance of high-heeled shoes with narrow toe
boxes.
proper shoe wear and the avoidance of high-heeled shoes with narrow toe
boxes.
FAQ
Q: When is bunion surgery indicated?
A:
Bunion surgery is indicated for painful lesions that have not responded
to nonoperative therapy, including trials of wide toe-box shoe wear.
Bunion surgery is indicated for painful lesions that have not responded
to nonoperative therapy, including trials of wide toe-box shoe wear.
Q: What can be done to prevent recurrence?
A: Avoidance of high-heeled, narrow toe-box shoe wear is critical to preventing recurrence.
