The Examination in Coma
coma or altered mental status is often complex and always urgent. The
neurologic examination is only one of several diagnostic methods that
can be brought to bear in coma; and imaging, cerebrospinal fluid (CSF),
and laboratory investigations play a vital role. However, the findings
on examination often determine the early management, and the urgency
with which imaging and CSF studies are obtained. Coma is a complicated
topic, and this discussion will focus on what can be learned from the
examination.
Arousal is a primitive function sustained by deep brainstem and medial
thalamic structures. Cognitive functions require an intact cerebral
cortex and major subcortical nuclei. In coma, stupor, and hypersomnia
there is a lowering of consciousness; in confusion and delirium there
is a clouding of consciousness.
system of fibers which arises from the reticular formation of the
brainstem, primarily the paramedian tegmentum of the upper pons and
midbrain, and projects to the paramedian, parafascicular, centromedian,
and intralaminar nuclei of the thalamus. Neurons in the reticular
formation also receive collaterals from the ascending spinothalamic
pathways and send projections diffusely to the entire cerebral cortex,
so that sensory stimuli are involved not
only
with sensory perception but—through their connections with the RAS—with
the maintenance of consciousness. The fibers in the RAS are
cholinergic, adrenergic, dopaminergic, serotonergic, and histaminergic.
Experimentally, stimulation of the RAS produces arousal, and
destruction of the RAS produces coma. The hypothalamus is also
important for consciousness; arousal can be produced by stimulation of
the posterior hypothalamic region.
structural or metabolic. Although restricted, focal lesions of the RAS
can produce profound alterations in consciousness; hemispheric lesions
cause coma only when extensive and bilateral, such as with head injury,
meningitis, encephalitis, or bilateral cerebral infarction. The degree
of alteration in consciousness is roughly proportional to the volume of
brain tissue involved in the process. Focal lesions restricted to
either hemisphere rarely produce significant alterations of
consciousness. Metabolic processes produce coma by diffusely affecting
the cerebral hemispheres or depressing the activity in the RAS, or both.
substrate, the initial management of coma, unless the cause is
immediately apparent, is directed toward correction of possible
deficiencies in glucose, oxygenation, and blood pressure; these
emergency measures are necessary, even before a detailed history and
examination. After initial determination of vital signs, attention
should first be directed toward ensuring an adequate airway and
oxygenation, blood pressure, and intravenous access. After obtaining
emergency blood samples, 50 cc of 50% glucose should be given, followed
quickly by 100 mg of thiamine IV in case the patient is alcoholic
(Wernicke encephalopathy can be precipitated by IV glucose in such
patients). Naloxone and flumazenil are often given empirically in case
there has been an opiate or benzodiazepine overdose. A “coma cocktail,”
consisting of dextrose, flumazenil, naloxone, and thiamine is sometimes
used in the initial management of the comatose patient. Because the
rapid reagent test strips used for glucose determination are not
infallible, studies favor empirical administration of dextrose and
thiamine to patients with altered consciousness, but naloxone should
probably be reserved for patients with signs and symptoms of opioid
intoxication, and flumazenil best left for reversal of therapeutic
conscious sedation and rare select cases of benzodiazepine overdose.
Preparations for intubation, respiratory support, and use of pressor
agents must be made, should they become necessary. Always assume a
cervical spine injury may be present, and immobilize the neck until a
fracture can be ruled out.
the central nervous system (CNS), a rapid neurologic examination should
be performed to search for obvious signs, such as a dilated pupil, that
may require urgent imaging and neurosurgical intervention. Otherwise,
the initial emergent management should be followed by a history and
general physical and neurologic examinations.
obtain, historical information is extremely important and well worth
pursuing vigorously. In the absence of family, a phone call to the
neighbor, landlord, or companion may yield valuable details about the
sequence of events leading to coma, the patient’s past health and
illnesses, and current medications. A history of known seizure
disorder, diabetes mellitus, hypertension, substance abuse, depression,
or suicide attempts may emerge. Check the wallet or purse for
medication lists, a doctor’s card or phone number, medical alert card,
or other pertinent information. Talk with police or ambulance drivers
if they are involved.
The patient should always be examined carefully for bruises and
hematomas, lacerations, fractures, and other signs of injury,
especially about the head. It is essential to remember that two
conditions may occur together (e.g., trauma and alcoholic
intoxication). Simple vital signs may provide important clues. An
elevated temperature suggests infection or serious intracranial
disease. Extremely elevated blood pressure suggests hypertensive
encephalopathy or subarachnoid hemorrhage. Hypotension suggests
impaired CNS perfusion due to some systemic process, such as hemorrhage
or myocardial disease. Hypotension rarely occurs because of primary CNS
disease, except in the terminal phase. Either tachycardia or
bradycardia may impair CNS perfusion. The combination of hypertension
and bradycardia suggests brainstem dysfunction, often because of
increased intracranial pressure (Cushing reflex).
evaluation of patients with depressed consciousness. Abnormal
respiratory patterns due to neurologic disease include Cheyne-Stokes
respirations (CSR), central neurogenic hyperventilation, ataxic
breathing, and apneustic breathing. In CSR, periods of hyperpnea
alternate with periods of hypopnea. Respirations increase in depth and
volume up to a peak, and then decline until there is a period of apnea,
after which the cycle repeats. In posthyperventilation apnea, a brief
period of hyperventilation is followed by apnea lasting 15 to 30
seconds or longer. The mechanisms underlying CSR and
posthyperventilation apnea are likely similar. Cheyne-Stokes
respirations may be due to bilateral hemisphere lesions, as well as to
increased intracranial pressure and cardiopulmonary dysfunction. In
respiratory ataxia, the pattern of breathing is irregular, with erratic
shallow and deep respiratory movements. Ataxic breathing occurs with
dysfunction of the medullary respiratory centers, and may signify
impending agonal respirations and apnea. Central neurogenic
hyperventilation refers to sustained, rapid, and regular hyperpnea. It
is primarily associated with disease affecting the paramedian reticular
formation in the low midbrain and upper pons, but it may also occur
with lesions in other brainstem locations, either intra-axial or
extra-axial. Apneustic breathing, which is rare, causes a prolonged
inspiratory phase, and occurs in pontine lesions just rostral to the
trigeminal motor nuclei, or cervicomedullary compression. Abnormal
respiratory patterns may occur because of systemic disease, such as
diabetic ketoacidosis (Table 35.1). Slow, regular respirations are noted with a variety of substance or drug intoxications and in severe myxedema.
age, grooming, and signs of acute or chronic illnesses such as fever,
cyanosis, jaundice, pallor, and signs of dehydration and loss of
weight. Assess responses to noises, verbal commands, visual stimuli,
threats, and tactile and painful stimulation, and whether there has
been incontinence. Note whether the patient, even in coma, appears to
be comfortable and natural or assumes unnatural positions. Carefully
observe spontaneous movements, and the reaction to various stimuli.
Note general activity (immobile, underactive, restless, or
hyperkinetic), tone (limp, relaxed, rigid, or tense), and the presence
of abnormal movements (tremors, twitches, tics, grimaces, and spasms).
Motor unrest and excessive activity are seen in both organic and
psychogenic states. If there is seizure activity, note the distribution
and pattern of spread of the convulsive movements, and any associated
manifestations such as the degree of impairment of consciousness,
frothing at the mouth, tongue biting, and incontinence.
and as often as necessary until the diagnosis is established. Note the
patient’s reactions to physicians, nurses, and relatives. Do the eyes
follow people? Is there some awareness of what is happening in the
immediate environment? The conduct may be constant or may vary from
time to time. For instance, the patient may appear to be completely
unconscious and fail to respond to any type of stimulation while the
observer is in the room, yet when not aware of being watched, may open
the eyes, make furtive glances, and move around.
|
TABLE 35.1 Findings on General Physical Examination that May Provide a Clue to the Etiology of Coma or Altered Mental Status
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
exam may help characterize the pathologic process. Specific attention
should be paid to the level of responsiveness, pupils, eye movements,
and motor responses.
states of disordered consciousness necessarily vary with the degree of
impairment and depth of coma. As a minimum, the following must be
assessed: level of consciousness, pupils, eye movements (including
reflex movements), fundoscopic, motor status, reflexes, and meningeal
signs. Other portions of the examination then follow as necessary. Coma
is most often due to a metabolic process. With rare exception,
metabolic
encephalopathies
are characterized by reactive pupils and a symmetric neurologic
examination. Any asymmetry in motor or sensory responses and any
pupillary or eye movement abnormality should prompt an immediate,
vigorous search for structural disease.
which the patient cannot be aroused by ordinary stimuli. There is
complete unresponsiveness to self and the environment. The patient in
coma has no awareness of herself, makes no voluntary movements, and has
no sleep-wake cycles. Stupor is a state of partial or relative loss of
response to the environment in which the patient’s consciousness may be
impaired to varying degrees. The patient is difficult to arouse, and
although brief stimulation may be possible, responses are slow and
inadequate. The patient is otherwise oblivious to what is happening in
the environment, and promptly falls back into the stuporous state. The
lethargic patient can usually be aroused or awakened and may then
appear to be in complete possession of her senses, but promptly falls
asleep when left alone. In a confusional state patients may be alert,
but are confused and disoriented. Patients with delirium are confused,
disoriented, and often agitated; the best example is delirium tremens.
Terminologic description of the differences between various states of
impaired altered consciousness is at best ambiguous. Because of
imprecision and inconsistency in usage, such terms as semi-coma and
semi-stupor, all describing changes across a spectrum of altered
awareness, are best avoided. It is preferable to describe the patient’s
state of responsiveness, or use an objective and well-defined scheme,
such as the Glasgow coma scale (GCS), which has gained wide acceptance
in the evaluation of patients with impaired consciousness, particularly
in head injury. In the GCS, scores are obtained for ocular, verbal, and
motor functions (Table 35.2). An alert person
with normal eye and motor responses would score 15 points; a patient in
profound coma would score 3 points. Other coma scales are available.
Coma must be distinguished from the persistent vegetative state,
locked-in syndrome, and mutism.
|
TABLE 35.2 The Glasgow Coma Scale
|
||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
||||||||||||||||||||||||||||||||||||||||||||||||||||
describe a variety of abnormalities of cerebral function. It is used
haphazardly to describe patients who have impaired alertness, impaired
cognition, or a deficit of higher cortical function. Strictly speaking,
the term AMS should imply a change in the level of consciousness,
somewhere on a continuum between confusion and coma. It should not be
used to describe patients who have impaired cognition with a clear
sensorium—those patients have dementia; patients who have focal
deficits of higher cortical function, such as aphasia; or used to
describe patients who have psychiatric disorders, such as psychosis or
mania. Neurologically naive clinicians may lump all these conditions
together under the rubric AMS. They are in fact distinctly different
conditions, with different etiologies and treatments, and especially
with different prognostic implications. Patients with Wernicke aphasia
are often thought to have AMS or an acute confusional state.
the patient, and this usually includes assessing the response to a
painful stimulus. Commonly used painful stimuli are supraorbital
pressure, sternal rub, and nailbed pressure. The stimulus must be
adequate but remain humane and considerate. Avoid leaving bruises or
other marks on the patient; the reason for these may be misinterpreted
by family members and ancillary personnel. An effective and stealthy
painful stimulus is to forcibly twist a key or the handle of a reflex
hammer between two fingers or toes squeezed tightly together.
in any detail in a patient with altered consciousness, examination of
the pupils and extraocular movements are critical in evaluation of the
comatose patient. The pupils are critical in the evaluation of altered
consciousness. The size, shape, position, equality, and reactivity are
all important. Bilateral pinpoint pupils occur with opiate toxicity and
other lesions of the pons, such as pontine hemorrhage or thrombosis of
the basilar artery. The bilateral miosis seen in large pontine lesions
is probably due to dysfunction of the descending sympathetic pathways
bilaterally. The light reaction is preserved with lesions involving the
descending sympathetic system, but may be very difficult to see without
magnification when the pupils are extremely small. Focusing on a tiny
pupil with the ophthalmoscope, and turning the light off, then back on,
may reveal the residual light reactivity. Hypothermia can cause small,
unreactive pupils. Bilateral large pupils in coma are usually an
ominous sign, especially when unreactive to light. They occur as a
terminal condition in many patients. Bilateral mydriasis may also occur
in botulism or anticholinergic intoxication. Midposition (3 mm to 6 mm)
unreactive pupils result from lesions affecting both sympathetic and
parasympathetic pathways. They occur commonly as a feature of central
transtentorial herniation.
disease. A unilaterally dilated pupil, especially if unreactive to
light, is most often a sign of third nerve palsy, and in the setting of
coma usually indicates uncal herniation. Because of the peripheral
location of the pupillary fibers in the third nerve, they are
especially susceptible to pressure, and pupillary dilation often occurs
prior to any eye movement abnormality. Coma with a unilaterally dilated
pupil could also result from subarachnoid hemorrhage due to a posterior
communicating artery aneurysm. Lateral medullary syndrome may cause
anisocoria due to Horner syndrome, along with evidence of brainstem
dysfunction, but rarely causes coma. Horner syndrome may also occur
with lesions involving the hypothalamus or thalamus (particularly
hemorrhage). Ipsilateral Horner syndrome may occur because of carotid
artery disease, especially occlusion, but is likely due to hypothalamic
ischemia rather than dysfunction of the pericarotid sympathetic plexus.
Rarely, seizures may cause transient anisocoria.
structural from metabolic coma. Normally reactive pupils in the setting
of coma suggest metabolic encephalopathy, which typically affects
consciousness and respiration earlier than pupillary function. Loss of
pupillary reactivity is more consistent with structural disease or
anoxia. Structural lesions of the brainstem usually cause
abnormal
pupillary responses, and in brain death pupillary responses are absent.
Pupillary reactivity is usually preserved in drug-induced coma, except
when extremely severe. A notable exception to the rule is that
posterior fossa mass effect exerted primarily on the mid and lower
brainstem, such as cerebellar infarction or hemorrhage, may initially
spare the pupils. Pupillary light reaction is a key prognostic sign.
Loss of reactivity portends a poor outcome. Brain injury patients, even
those with a GCS of 3, if the pupils remain reactive, may survive. The
ciliospinal reflex is another test of pupil reactivity, but it involves
pathways caudal to the foramen magnum.
reflexes should be examined carefully. Note the position of the eyes at
rest, whether there is any nystagmus, and whether the range of ocular
movement is full in both directions to passive head movement or
oculovestibular stimulation. If there is any possibility of trauma, a
cervical spine series should precede neck manipulation for eye movement
examination. Roving eye movements indicate that brainstem function is
intact. Conjugate eye deviation away from the paralyzed extremities is
seen in destructive frontal lobe lesions; conjugate deviation in the
direction of the paralyzed extremities indicates a brainstem lesion.
Conjugate gaze deviation, sometimes with accompanying nystagmoid
jerking, may also occur because of seizure activity in the frontal eye
fields on the side the patient is looking away from. Thalamic
hemorrhage can cause “wrong-way eyes,” with gaze deviation toward the
hemiparesis. Vertical gaze deviations suggest brainstem disease; the
most common is sustained downgaze with an upgaze deficit due to a
lesion involving the upper midbrain or caudal thalamus. Hepatic
encephalopathy can cause down-gaze deviation.
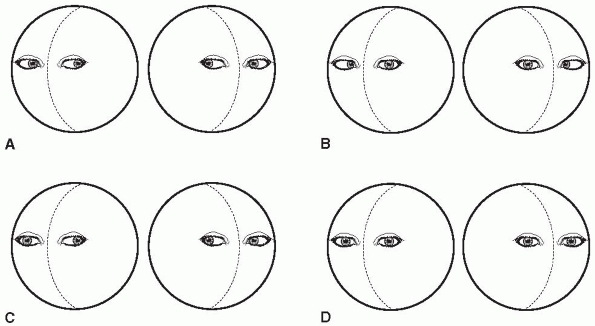
to side (doll’s eye movements, oculocephalic reflex) or by the
injection of ice water into the external auditory canal (caloric test,
oculovestibular reflex) may reveal isolated weakness of particular
extraocular muscles, gaze paresis, or other eye movement abnormalities (Figure 35.1).
Supratentorial lesions and metabolic processes usually do not affect
the oculocephalic reflex. Caloric testing assesses the same brainstem
reflexes as the doll’s eye maneuver, and is used if the oculocephalic
reflex is not intact. After ensuring the external auditory canal is
clear, the head is flexed to a 30-degree angle above horizontal and 10
cc to 20 cc of ice water is instilled into the canal. If no response is
obtained, larger volumes are used.
After
15 to 60 seconds, eye deviation begins and may last several minutes.
The expected response in coma is tonic deviation of the eyes toward the
side of the irrigated ear. Warm water causes the opposite response.
Testing of the other side may be done after about 5 minutes. Brainstem
lesions affecting the pathways and nuclei subserving the reflex may
cause an abnormal response. In coma, absence of a response to cold
calorics suggests sedative hypnotic drug intoxication, a structural
lesion of the brainstem, or brain death, unless there is evidence of a
vestibular disorder or exposure to vestibular-suppressant drugs. When
the response is present, the eye movements may be dysconjugate. Some
drugs, particularly sedative-hypnotic agents, tricyclics, and
anticonvulsants, may affect eye movements in a comatose patient.
Unusual spontaneous eye movements may occur in coma (e.g., ocular
bobbing, ping-pong gaze), and the particular pattern often has
localizing significance. If the patient is responsive enough, testing
for optokinetic nystagmus may give important diagnostic information.
 |
|
FIGURE 35.1
• Examples of oculocephalic responses that may be seen in comatose patients. When the brainstem is intact, the eyes move in the opposite direction from head rotation. A. Normal response, the usual response in a patient with metabolic encephalopathy. B. Bilateral sixth nerve palsies. C. Right third nerve palsy or internuclear ophthalmoplegia. D. Absent response, seen when the reflex pathways are impaired. |
of the palpebral fissures on the two sides. When the eyelids are closed
in a comatose patient, the lower pons is still functioning. Asymmetry
of the palpebral fissures may indicate either upper facial weakness on
the side of the wider fissure, or ptosis on the side of the narrower.
If the eyes are partially or completely closed, the examiner may try to
open them by gently raising the upper lids, and then noting the speed
with which the eyes close again. Unilateral orbicularis weakness may
produce more leisurely closure on the affected side. In deep coma, the
eyes may be open and a glassy stare evident. In profound illness, the
patient often lies with the eyes only partially closed, even in sleep,
so that a narrow portion of the cornea is visible between the upper and
lower lids. In psychogenic unresponsiveness (hysterical coma), the
patient may keep the eyes tightly closed and resist attempts to open
them, yet open the eyes and glance around when unaware that someone is
observing the action. Note whether there is any blinking, flickering,
or tremor of the eyelids at rest or in response to a bright light or
sudden noise. The corneal reflexes may be absent in coma; any asymmetry
of the response may be significant.
movement by painful stimulation, such as supraorbital pressure, sternal
rub, or pinprick stimulation of the face. The area of the upper
nasolabial fold at the junction with the nose is particularly sensitive
and a response to pinprick in this region can sometimes be obtained
when there is no response over other parts of the face. It is important
when examining facial sensation not to traumatize the face and leave
pinprick marks, particularly in elderly patients with thin, fragile
skin. Firm manual pressure over the supraorbital notch, at the point of
emergence of the supraorbital nerve, will often produce facial
grimacing. When facial movement does occur, compare the two sides for
symmetry of the response. Elicitation of a blink response to loud noise
provides a crude assessment of auditory function. The mouth may be
either open or closed. In nonorganic unresponsiveness the patient may
resist attempts to passively open the mouth. A gag reflex may or may
not be present. If present, the palate should rise in the midline.
consciousness is complete without an ophthalmoscopic examination. The
presence of papilledema is, of course, indicative of some process
causing increased intracranial pressure. Papilledema takes a period of
time to develop, and may be absent in acute conditions. Normal
spontaneous venous pulsations are a strong indicator of normal
intracranial pressure, but absence of venous pulsations does not prove
intracranial pressure is increased. Subarachnoid hemorrhage may produce
subhyaloid hemorrhages in the retina. The ophthalmoscopic examination
is also important in detecting systemic diseases responsible for
altered consciousness (e.g., diabetes, hypertension, or endocarditis).
It is not possible to test either visual acuity or the visual fields
reliably if significant impairment of consciousness is present. If the
patient is responsive enough it may be possible to determine if the
patient follows objects, or blinks to threat.
requires skilled observation. It may be difficult to recognize the
presence of a hemiplegia in a comatose patient. If the hemiplegia has
been of sudden onset, the paralyzed side of the body is usually
flaccid. The width of the palpebral fissure is increased,
the
nasolabial fold is shallow, and the angle of the mouth droops on that
side. There may be drooling of saliva and puffing out and retraction of
the cheek on expiration and inspiration. If both arms are lifted, or
placed with the elbows resting on the bed and the forearms at right
angles to the arms, then released by the examiner, the affected
extremity falls more rapidly and in a flail-like manner, while the
normal arm drops slowly, or may even remain upright for a brief period
before falling. If the lower extremities are lifted from the bed and
then released, the affected extremity falls rapidly, while the normal
limb drops more gradually to the bed. If the lower extremities are
passively flexed with heels resting on the bed and then released, the
paretic limb rapidly falls to an extended position with the hip in
external rotation, while the unaffected limb maintains the posture for
a few moments and then gradually returns to its original position. If
the depression of consciousness is not too deep, there may be some
response to painful stimulation. Pinching the skin on the normal side
is followed by withdrawal of the part stimulated. In contrast, a
painful stimulus on the paralyzed side causes no local movement,
although grimacing or movements of the opposite side of the body may
indicate that some sensation is retained. Other tests of motor
function, such as evaluation of coordination and active movement,
cannot be performed on unresponsive patients. It is important to
appraise muscle tone, or resistance to passive movement, and to observe
carefully for any abnormal movements. Occasionally, spasticity instead
of flaccidity develops after acute cerebral lesions. A previous spastic
hemiplegia or extrapyramidal syndrome may have caused an alteration in
tone that persists even in coma, and arthropathies and skeletal
abnormalities may also interfere with joint movements. In catatonia
there may be a waxy resistance resembling that of extrapyramidal
disease. Patients with AMS may have asterixis.
important factor in gauging the depth of coma and prognosis. The
highest level response is when the patient obeys simple commands (GCS
6). If there is no response to verbal commands, a painful stimulus is
delivered. There are five possible outcomes. The patient may localize
the painful stimulus and make appropriate movements to attempt to
remove it (GCS 5). She may exhibit flexion withdrawal without
localizing the stimulus (GCS 4). There may be abnormal flexor responses
(decorticate rigidity, GCS 3), or, as the lowest level of response, an
extensor response (decerebrate rigidity, GCS 2). The worst possible
outcome is no response whatsoever (GCS 1).
as posturing. Abnormal posturing may occur spontaneously, as well as in
response to stimuli. It is not uncommon for posturing to be different
on the two sides of the body. When there is difficulty distinguishing
purposeful withdrawal from decorticate posturing, a painful stimulus to
the inner arm is useful. Abduction of the arm away from the stimulus is
a high-level avoidance response; adduction into the stimulus is a
low-level reflex response. Posturing usually indicates structural
disease of the nervous system, and is particularly common after head
injury. Posturing can also occur with severe metabolic encephalopathy,
particularly sedative-hypnotic drug intoxication.
perceive even the most painful stimulus, or may respond to painful
stimuli by wincing and withdrawing the part of the body stimulated.
Often, the examination must be limited to comparing responses to
painful stimulation on the two sides of the body. Sensory stimuli may
be delivered by pinching the skin, pricking with a sharp object,
pressing over the supraorbital notch, and squeezing the muscle masses
and tendons, particularly the Achilles tendon.
plantar responses should be tested. Frontal release signs (forced
grasping, palmomental, and suck or snout responses) and paratonic
rigidity may be present with AMS of either structural or metabolic
origin. Asymmetry of responses may have some localizing value.
Similarly, extensor plantar responses may occur with either structural
or metabolic coma.
involvement by flexing the neck passively and rotating it from side to
side in order to detect nuchal rigidity. The Kernig, Brudzinski, and
related signs may be absent in some cases of deep coma despite the
presence of meningeal irritation. In subarachnoid hemorrhage, it
requires some hours for meningeal signs to develop, and they may be
absent at the time of presentation.
primary CNS disease, (b) depression of the CNS by a systemic metabolic
process or drug intoxication, and (c) psychogenic unresponsiveness.
Statistically, the most likely etiology is involvement of the CNS by a
systemic metabolic process or drug intoxication. Patients with
metabolic encephalopathy characteristically have a symmetrical
examination, devoid of lateralizing or focal abnormalities, intact
reflex eye movements, and reactive pupils.
may cause coma: (a) a lateralized hemispheric mass lesion causes
increased intracranial pressure, herniation, and compression or
hemorrhage into the upper midbrain with secondary impairment of the
RAS; (b) a brainstem lesion, such as hemorrhage or infarction, damages
the RAS directly; and (c) a disease process affects both cerebral
hemispheres, or both hemispheres and the RAS. The findings with a
hemispheric mass lesion depend upon the stage of evolution of the
process. In the early stages, there are usually lateralizing findings
and asymmetries on examination consistent with a focal process. These
include hemiparesis, focal seizures, aphasia, hemianopia, apraxia, and
other signs of hemispheric dysfunction. As the lesion expands and
intracranial pressure increases, the other hemisphere becomes involved,
herniation develops, and the focal nature of the process becomes
complicated by findings due to herniation. Asymmetric motor responses
and abnormal eye movements usually persist until the terminal stages.
Herniation syndromes are due to shifting of brain structures caused by
increased intracranial pressure. They are evidence of severe disease,
and are life-threatening. A number of different herniation syndromes
have been recognized. The more common and important are central
transtentorial, lateral transtentorial (uncal), and tonsillar (foramen
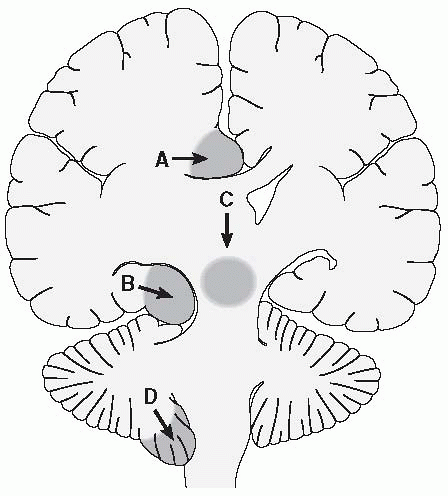
magnum) herniation (Figure 35.2, Table 35.3).
 |
|
FIGURE 35.2 • Patterns of brain herniation. A. Herniation of the cingulate gyrus under the falx cerebri. B. Uncal (lateral transtentorial) herniation. C. Central transtentorial herniation. D. Herniation of the cerebellar tonsils through the foramen magnum.
(Reprinted with permission from Wilkins RH, Rengachary SS. Neurosurgery. New York: McGraw-Hill, 1985.)
|
|
TABLE 35.3 Clinical Manifestations of Common Herniation Syndromes
|
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
|
downward displacement of the hemispheres causing impaction of the
diencephalon and midbrain into the tentorial notch. Pressure effects on
the diencephalon and midbrain often cause small hemorrhages in the
upper midbrain (Duret hemorrhages). Uncal herniation occurs when the
temporal lobe and uncus shift medially into the tentorial notch,
causing compression of the third cranial nerve and adjacent midbrain.
Tentorial herniation, unless reversed, evolves into an orderly
progression of neurologic dysfunction referred to as rostrocaudal
deterioration.
dysfunction becomes progressively more dramatic. Clinical stages occur
as if the brain had been transversely sectioned at a particular level
(diencephalon, midbrain, pons, or medulla). Respirations become
progressively more abnormal, evolving from a Cheyne-Stokes pattern
early, to ataxic respirations to eventual apnea. Pupils become
progressively more abnormal and eventually become fixed and unreactive.
Reflex eye movements are eventually lost. Motor responses evolve from
localizing to nonlocalizing to decorticate to decerebrate to flaccid.
The end result of unchecked rostrocaudal deterioration is death.
foramen magnum compresses the medulla and upper spinal cord, and can
result in rapid failure of vital functions. A dreaded complication of
lumbar puncture is herniation, especially cerebellar tonsillar
herniation, due to removal of spinal fluid.
hemorrhage or infarction) produces coma that is abrupt in onset, and
causes focal or multifocal abnormalities, abnormal eye movements,
pupillary abnormalities, pathologic reflexes, abnormal posturing, and
other objective neurologic signs.
or produce diffuse CNS involvement include bilateral subdural
hematomas, bilateral cerebral infarction due to emboli, and other
processes that may cause multifocal lesions. In addition, some
processes affect the CNS in a more diffuse or widespread manner and
cause coma by dysfunction of the cerebral hemispheres bilaterally or
the cerebral hemispheres as well as the RAS. Such conditions include
meningitis, encephalitis, and subarachnoid hemorrhage. These cause
variable focality on examination, depending on the specifics of the
process, and occasionally cause very little in the way of focal or
lateralizing signs. There typically are objective neurologic signs in
the form of reflex abnormality, pathologic
reflexes,
evidence of meningeal irritation, and abnormalities on fundoscopic
examination. In addition, there may be fever or other evidence of
systemic disease.
produce no focal or lateralizing signs on neurologic examination,
preserved pupil reactivity, and usually do not affect eye movements or
cause other signs of brainstem dysfunction. Metabolic encephalopathy
often begins with a period of confusion or delirium, which gradually
evolves into stupor, then coma. There are three common etiologies: (a)
intoxication, (b) severe systemic metabolic disturbance, and (c)
systemic infection. Intoxication is usually due to alcohol, opiates, or
sedative-hypnotic drugs. These conditions sometimes produce other
abnormalities on physical examination that may be a clue as to
etiology, such as pinpoint pupils, respiratory depression, or skin
lesions.
coma is the hypoxic-ischemic encephalopathy that follows cardiac
arrest. Other examples include hypoglycemia, diabetic ketoacidosis,
nonketotic hyperosmolar state, hyperammonemia, hypercalcemia, and
hypercarbia. Many of these conditions occur under obvious clinical
circumstances, such as known diabetes, end-stage alcoholism with
cirrhosis, or severe pulmonary disease with hypercarbia, and the
etiology is often revealed by routine blood chemistries. Severe
infections and septicemia occasionally cause altered mental status
(septic encephalopathy).
uniform clinical picture of a symmetric examination with reactive
pupils and intact brainstem eye movement reflexes, in some conditions
there may be deviations from this scheme. Occasionally, certain
clinical features may provide clues as to etiology. In hypoglycemia
there may be lateralized deficits, extensor posturing, hypothermia, and
seizures. In hepatic encephalopathy there may be clinical evidence of
alcoholism and end-stage liver disease, including ascites, jaundice,
spider angiomas, palmar erythema, and gynecomastia. It is usually
preceded by asterixis and confusion. There may be focal deficits, as
well as abnormal posturing, and occasionally unusual eye findings,
including ocular bobbing and gaze deviations. The encephalopathy of
uremia is often associated with tremor, asterixis, myoclonus, seizures,
and occasionally evidence of tetany. There may be mild focal deficits,
but brainstem functions remain intact. Distinguishing features of the
encephalopathy of hypercarbia include papilledema, asterixis, tremor,
and myoclonus. Focal signs occur occasionally in hyponatremia,
hypernatremia, and hyperosmolar coma. Sedative-hypnotic drug
intoxication often affects eye movements, while pupillary light
reactions remain unaffected. Abnormal posturing may also occur. This
unusual combination of reactive pupils in the face of abnormal reflex
eye movements and posturing is characteristic of sedative-hypnotic drug
effects, but can also occur with posterior fossa mass lesions causing
pressure on the lower and mid-brainstem with relative preservation of
the midbrain. This picture can also occur with upward transtentorial
herniation.
activity, focal or generalized, usually accompanied by clouding or loss
of consciousness. In addition to alteration of consciousness during the
ictus, seizure disorders may also cause AMS due to postictal
unresponsiveness, absence status, psychomotor status, and subclinical
status epilepticus. In the postictal period there is often depression
of consciousness, a desire to sleep, confusion, and disorientation.
Coma or stupor may be a sequel of a recent seizure, although it may not
be possible to obtain a history of either a recent convulsion or
previous attacks. The patient may show evidence of tongue-biting,
frothing at the mouth, bloody sputum, incontinence, and lacerations or
other injuries to the body. Old scars may be found on the tongue. The
postictal stupor is usually brief, but may be followed by either
profound sleep or confusion and irrational behavior. A prolonged
postictal encephalopathy may last many hours, rarely days. Postictal
stupor occurs most commonly with generalized tonic clonic seizures, but
may follow other seizure types. In the absence of a history of seizure
disorder, it may be difficult to differentiate between the postictal
state and cerebral trauma.
activity, or repeated convulsions with failure to regain consciousness
between them. Status epilepticus may cause a state of altered
consciousness that may be confused with AMS or coma. In absence (petit
mal) status there is lowering and clouding of consciousness and the
patient may appear to be in a trancelike stupor suggesting drug abuse
or a psychiatric disorder. Patients in complex partial status
epilepticus are commonly confused or lethargic. Subclinical status
epilepticus, or seizures with subtle motor manifestations, may cause a
coma-like state. Subclinical status may continue in patients when the
motor manifestations have been suppressed with antiepileptic drugs.
Patients with pseudoperiodic lateralized epileptiform discharges
(PLEDs) are often comatose because of a hemispheric process, such as
large infarction or subdural hematoma; and the electroencephalogram
demonstrates characteristic discharges. The presence of myoclonus
usually indicates that coma is of metabolic origin. Spontaneous,
multifocal myoclonic jerking is common, particularly in uremia and
hypercarbia. Massive generalized myoclonic jerks often occur as an
aftermath of cardiac arrest and cerebral anoxia, and are an extremely
poor prognostic sign.
sparing the RAS renders the patient mute and quadriplegic but not
comatose. There is complete paralysis of all four extremities and the
lower cranial nerves but no associated impairment of consciousness.
Patients with locked-in syndrome have quadriplegia and anarthria, but
variable preservation of consciousness and intellect. The patient is
awake but speechless and motionless, with little response to stimuli.
The lesion usually involves the midpons and results in paralysis of
facial movement and horizontal gaze. If the supranuclear vertical gaze
pathways, which pass rostral to the other corticobulbar and
corticospinal pathways, are spared there is preservation of vertical
eye movements and the patient may be able to blink. With effort,
communication may be established using eye movement or blink signals.
Sensory pathways, hearing, and vision are largely spared, and the
patient is effectively “de-efferented.” Other findings vary with the
particulars of the lesion. A fulminant neuropathy, such as
Guillain-Barré syndrome, can result in a clinical state resembling
brain death through diffuse de-efferentation. Jean-Dominique Bauby
(deceased) bequeathed an eloquent and poignant description of the
locked-in state from the victim’s point of view in The Diving Bell and the Butterfly: A Memoir of Life in Death
(Vintage Books, 1998). Bauby dictated his book by blinking one eyelid.
The principal cause of locked-in syndrome is brainstem stroke (86%),
but it may also occur after trauma (14%). The locked-in state is
frequently mistaken for coma. Appreciation that the patient is not
comatose or vegetative but locked-in does not usually occur for 2 to 3
months (mean 79 days), and the average survival locked-in is 71 months.
state (PVS) invariably entails massive bilateral hemispheric damage
with a spared and intact brainstem. Preservation of the RAS permits
behavioral arousal and sleep wake cycles, but existence is devoid of
cognition. Positron emission tomography has demonstrated cerebral
metabolic rates for glucose far too low to sustain consciousness. The
PVS may develop as a sequel to acute insults, typically following a
temporary period of coma, or as the end stage of a progressive
neurologic illness, such as Alzheimer disease.
seemingly alert demeanor, they display no speech, comprehension, or
purposeful movement. Reflex eye movements and orientation to
noise—brainstem level functions—may persist. Yawning, sneezing,
bruxism, and occasional meaningless smiles may occur. Impaired motor
function with spasticity, posturing, or contractures is common. Painful
stimuli evoke nonspecific erratic reactions without discrete motor
responses or localization. All patients are incontinent of stool and
urine. In PVS, patients exist in eyes-open permanent unconsciousness,
with intact sleep-wake cycles but no awareness of self or environment,
and
without voluntary action or behavior of any kind. Though seemingly
awake, they display no interactive behavior and no ability to express
emotion or engage another person on any level. Extended observation
forms the primary and most important basis for the diagnosis of PVS.
Such patients show no behavioral responses whatsoever over a prolonged
period of time. Persistent vegetative state must be differentiated from
catatonia and from the locked-in syndrome.
states of altered awareness that are similar, if not identical, to PVS
(e.g., akinetic mutism, abulia, apallic state, coma vigil, and
pseudocoma). Much of the nomenclature is outdated and perplexing, the
distinctions vague and of marginal clinical utility.
hysteria or malingering, the loss of consciousness is typically not
deep, but the condition may occasionally simulate real coma. The
patient often responds to painful stimuli, unless there is associated
nonorganic sensory loss, and the reflexes are normal, with no
pathologic responses. The temperature, pulse, respirations, and blood
pressure are normal. The eyelids may flutter or the eyes may be closed
tightly with the patient resisting attempts to open them. The vigorous
eye closure may interfere with testing the corneal and pupillary
reflexes, which are normal. When the eyelids are opened and then
released by the examiner, they close gradually in the patient with real
coma but quickly in the patient with factitious coma. The patient may
resist other procedures, and glance around when unaware she is being
watched. When a hand is raised and allowed to drop toward the face, the
patient with psychogenic unresponsiveness will usually avoid hitting
herself, but this rule is not infallible. In true coma, the hand will
hit the face. Caloric testing produces nystagmus, which never occurs in
real coma.
precipitated by emotional stress, and the onset is often dramatic. The
patient may appear to be in a trance, or coma may alternate with
weeping and thrashing movements. The performance is appropriately
staged, and occurs when observers are in the vicinity. Movements, if
present, are not stereotyped, but appear to be coordinated and
purposive. The patient may struggle, clutch at objects or parts of the
body, or attempt to tear off clothes. Although the patient appears to
be unconscious, some response to external stimuli may be evident. If
there is muscle hypertonicity, it is usually of a rigid type, and there
may be opisthotonos with the arc de cercle. If the patient can be
persuaded to talk, the responses may be of the type seen in Ganser
syndrome, with evasiveness and approximate but consistently inaccurate
replies.
consciousness. Severe depression, schizophrenia, and organic psychoses
may cause mutism, in which the patient is either completely withdrawn
from the environment or refuses to speak. Negativism, either passive or
active, may be a symptom of various psychoses, but especially of
schizophrenia. In severe depression the patient may show psychomotor
retardation that may simulate AMS. In catatonic stupor there is apathy,
mutism, and negativism, often with waxy rigidity of the extremities
causing the patient to hold her limbs or entire body in bizarre and
seemingly uncomfortable positions for long periods of time. Food may be
held in the mouth.
of certainty regarding the etiology of the brain death picture is
imperative. Common causes include cerebral anoxia, cerebral hemorrhage,
aneurysmal subarachnoid hemorrhage, and head injury. The patient must
have no evidence of cerebral or brainstem activity, although segmental
reflex activity mediated at the spinal cord level may persist.
Preserved spinal cord reflex activity may lead to dramatic movements,
such as the “Lazarus reflex.” There may even be respiratory-like
movements, with shoulder elevation and adduction, back arching, and
intercostal expansion, but without significant tidal volumes. Deep
tendon reflexes, superficial reflexes, and the Babinski sign may be
present and do not countermand a diagnosis of brain death. Except for
segmental reflexes, motor responses are absent. The pupils
are
fixed, and oculocephalic and oculovestibular reflexes are absent, even
with large volume ice water caloric testing. There must be no evidence
of sedative drug effects or any systemic metabolic abnormality severe
enough to produce the clinical picture of brain death. There must be no
significant hypothermia, as hypothermia can mimic brain death. The
presence of neuromuscular blocking agents obviously precludes
evaluation of motor status. If the patient meets these clinical
criteria, an apnea test is performed, and if there is no respiratory
effort with an arterial PCO2 of 60 mm Hg or more, the diagnosis of
brain death can be made. The apnea test is not without danger. Dramatic
spontaneous movements are most likely to occur during the apnea test
when the patient becomes hypoxic. These clinical conditions should
persist for some time, the exact interval depending on the specific
circumstances. A repetition of the evaluation is often done to confirm
the findings; there is no decreed interval, but 6 hours is reasonable.
These criteria apply to adults and may have to be modified for
children, especially neonates.
|
TABLE 35.4 Summary of the Diagnostic Criteria for the Clinical Diagnosis of Brain Death from the American Academy of Neurology
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
practice parameter on determining brain death in adults prepared by the
Quality Standards Subcommittee of the American Academy of Neurology.
